
How to Live to 117: Lessons from the World’s Oldest Woman
The topic of longevity has become increasingly popular amongst scientists, and recent books dealing with longevity have become NYT bestsellers.
Partially fueled by this new effort to increase the human lifespan into the 100s, has been the emergence of biohackers and influencers promoting a litany of unsubstantiated intervention, without any scientific evidence. Even though I have often covered this topic in our newsletter and in podcasts, I thought a recent, unique study about this topic is worth discussing.
When Maria Branyas Morera passed away in August 2024, she was 117 years old, the oldest living person on Earth. Unlike many of us imagine old age, she didn’t spend her last years bedridden or cognitively impaired. She read books, gardened, played piano, enjoyed yogurt and olive oil, walked daily, and kept the company of friends and dogs. Her life was quiet, but her healthspan, the years she lived free from major disease, was extraordinary.
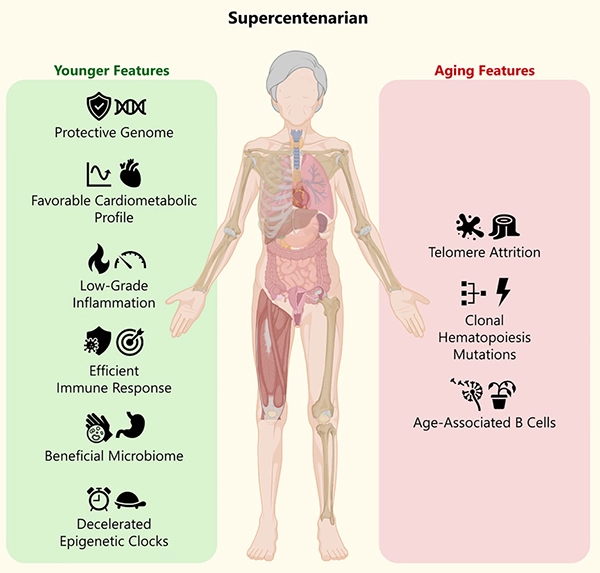
Winning the Genetic Lottery, But Not Entirely by Chance
Serious longevity researches like Eric Verdin, MD (see my podcast episode with him here) have always emphasized that genes are becoming more important at the extreme end of the spectrum, e.g. for those people living into their 100s. There’s no question that genetics also played a role in Morera’s exceptional longevity. Her genome carried multiple variants previously associated with long life, genes involved in DNA repair, mitochondrial efficiency, and the ability to clear damaged cells. These mechanisms prevent the accumulation of cellular waste and chronic inflammation, both of which accelerate biological aging.
Interestingly, she also carried seven new genetic variants that had never before been associated with extreme longevity. Just as important, she lacked the usual risk variants for Alzheimer’s disease, cancer, and diabetes. Her only chronic complaint was arthritis.
But Esteller’s team quickly realized that her genome alone couldn’t explain her 117 years. None of her relatives which shared many of her genes lived anywhere near that long. Something else, or rather, a combination of many “somethings”, was protecting her body and brain from decline.
An Immune System That Aged Gracefully
As we age, our immune systems typically decline, a process called immunosenescence and occurring in all of us. We lose the ability to mount strong responses to infection while becoming more prone to chronic inflammation and autoimmunity. Morera seemed to escape this fate.
Her blood contained an unusually large and functional population of memory T-cells, the immune soldiers that “remember” past infections and respond efficiently to new ones. She had fought off numerous infections during her lifetime, including COVID-19 at age 113, and recovered. Her immune system stayed “calm but ready,” not demonstrating the exaggerated immune responses seen in many patients with the most severe symptoms, highest death rate and greatest likelihood to develop long COVID.
Such a balanced response to perturbations has been referred to as biological resilience: the ability of the body’s regulatory systems, including the immune, nervous, and endocrine systems, to respond flexibly to stress without tipping into chronic inflammation or disease.
The Microbiome Connection
One of the most fascinating aspects of Esteller’s study was the analysis of Morera’s gut microbiome, the trillions of microorganisms living in the intestinal tract that interact closely with the immune system and the brain. Her microbiome was rich in bacteria known to produce anti-inflammatory metabolites, particularly short-chain fatty acids such as butyrate, which help regulate immune balance, and energy metabolism in the gut, the brain and may other organs.
Even at 116, her microbial diversity resembled that of a much younger person. This balance likely supported her immune efficiency and metabolic health. As I have discussed extensively in my book The Mind-Gut Immune Connection, the context of the brain-gut microbiome system, the resilience of her microbial ecosystem may have buffered her body and mind against the effects of chronic stress and accelerated aging.
It’s worth noting that Morera’s diet was simple but aligned with what research consistently links to a healthier microbiome: a traditional Mediterranean pattern with at least 70% of her diet being plant based. She ate lightly, three yogurts a day, plenty of olive oil, fish, fruit, and vegetables, with minimal processed foods. Yogurt, of course, provides live bacterial cultures, but the foundation of her microbiome health came from her lifelong pattern of eating whole, plant-based foods, the optimal diet for the gut microbiome.
Aging Without Illness
Physiologically, Morera showed signs of aging, her joints hurt, and her cells contained some abnormal proteins and blood markers that might have predicted disease. Yet she remained mentally sharp and physically functional. Her biological age, as measured by molecular markers, was estimated to be 23 years younger than her chronological age.
This distinction between aging and disease is critical. As Esteller put it, “Aging and illness are separable.” We tend to conflate the two, assuming that old age must come with frailty and dementia. The assumption that the prevalence of Alzheimer’s disease will automatically go up with the aging of the population is based on this mistake. Morera’s biology suggests otherwise: it’s possible to age, even to extreme old age, without developing chronic disease.
Her case supports a growing view in longevity research that maintaining physiological integration, the synchronized functioning of multiple body systems which all interact with each other, is more important than trying to “stop” aging at the cellular level, the popular approach by longevity gurus and biohackers. When the immune, metabolic, and microbial systems remain in balance, the body can stay resilient even in advanced age.
Lifestyle, Connection, and the Rhythms of Simplicity
Morera’s life was unhurried. She valued rest, relationships, nature, and music. She slept well, gardened regularly, and interacted with fellow residents in her assisted living community. These activities may seem mundane, but they mirror lifestyle patterns seen across “Blue Zones”, the regions of the world with the highest concentration of centenarians, such as Sardinia, Okinawa, and Ikaria.
Each of these cultures shares key features: mostly plant-based diets rich in polyphenols, regular low-intensity movement, strong social ties, and a sense of purpose. These are not “biohacks” but ways of living that align our circadian rhythms, stress physiology, and microbiome with the natural environment, what I often describe in my books as living in synchrony with the interconnected ecosystems within and around us.
Morera embodied this rhythm intuitively. She enjoyed the small pleasures of daily life and avoided excess, whether in food, stress, or ambition. That balance likely influenced everything from her insulin sensitivity to her gut microbial composition to the regulation of her stress-response systems.
What Can We Learn from Maria Branyas Morera?
Of course, we can’t all inherit her genes. But her story highlights that longevity is not a fluke. It’s the cumulative outcome of genetic potential expressed through lifestyle, environment, and social context. From the perspective of the brain-gut-microbiome system, several key lessons emerge:
1. Nourish your microbes.
A diverse, fiber- and polyphenol-rich diet, like the Mediterranean pattern, supports bacteria that produce anti-inflammatory molecules and help regulate immunity.
2. Maintain gentle, consistent movement.
Regular walking, gardening, or any low-intensity physical activity improves metabolic flexibility and promotes microbial diversity.
3. Prioritize social connection and purpose.
Social isolation is a form of chronic stress that disrupts the microbiome and accelerates immune aging. Morera stayed connected, curious, and kind.
4. Cultivate emotional and physiological balance.
Chronic stress accelerates cellular aging through cortisol and inflammatory signaling. Mindfulness, music, and time in nature buffer against this.
5. Eat lightly and simply.
Morera’s modest diet likely supported metabolic health and avoided chronic overnutrition, which drives insulin resistance and inflammation.
6. Respect the natural rhythm of life.
Adequate sleep, exposure to natural light, and daily routine help synchronize the body’s circadian systems, key regulators of immune and metabolic function.
The Science and the Soul of Longevity
While Esteller’s study offers a molecular portrait of one remarkable life, it also reminds us that science can only measure part of the story.
Morera’s longevity wasn’t just a triumph of DNA or diet, it was the result of a harmonious relationship between her biology and her environment. She lived with curiosity, gratitude, and balance.
As Esteller concluded, Maria Branyas Morera grew old, but she didn’t grow sick. Her body aged slowly, her mind stayed clear, and her spirit remained engaged. In the end, she died peacefully in her sleep, not from disease, but simply because her biological clock had run its natural course.
That, perhaps, is the most profound lesson of all: that longevity is not about fighting age but about living well within it, caring for the interconnected systems that sustain us, from our cells to our microbes to our communities.

Emeran Mayer, MD Is a Distinguished Research Professor in the Departments of Medicine, Physiology and Psychiatry at the David Geffen School of Medicine at UCLA, the Executive Director of the G. Oppenheimer Center for Neurobiology of Stress and Resilience and the Founding Director of the Goodman-Luskin Microbiome Center at UCLA.