
How the Gut Microbiome and Brain Team Up to Build Resilience to Stress
While stress has always been a feature of human life, chronic stress has progressively increased during the last 75 years—from job competition and financial pressures to increasing worries about the future of the world and the planet, to name just a few. But not everybody reacts to environmental stresses the same way, with some people being hyperresponsive to stress, while others demonstrate remarkable stress resilience. But why do some people bounce back from stress better than others? What makes someone resilient? A groundbreaking study from UCLA researchers shows that one of the key players in this process might be your gut and its microbes.
Research from a team of investigators at the UCLA Center for Neurobiology of Stress and Resilience found that people who are more resilient to stress have unique patterns in their gut microbiome—the trillions of bacteria living in your digestive system—and in how their brain functions. These differences may help protect them from anxiety, depression, and other stress-related health issues.
What Is Resilience—and Why Does It Matter?
Resilience is the ability to recover from difficulties. People who are resilient adapt better to stress, tend to have stronger emotional regulation, and are less likely to develop anxiety or depression. But resilience isn’t just a mindset—it also involves biological factors, like how your brain and gut interact, and as the new research shows, includes also your gut microbes.
The Brain–Gut Microbiome System
This study by Delgadillo and An, and published in the prestigious journal Nature Mental Health, focused on the brain–gut microbiome (BGM) system, a complex communication network between your brain, your gut and its microbiome. While past focus has been on the digestive functions of the gut, new research has demonstrated that this system plays a role in emotion regulation, well-being, mental focus, and stress responses. Disruptions in this system, due to changes in diet, lifestyle factors and chronic stress have been linked to a wide range of chronic conditions, including depression, anxiety, autism spectrum disorders and neurodegenerative syndromes. In this study, researchers wanted to know: Can the gut microbiome and brain patterns help explain why some people are more resilient to such disruptions?
The Study at a Glance
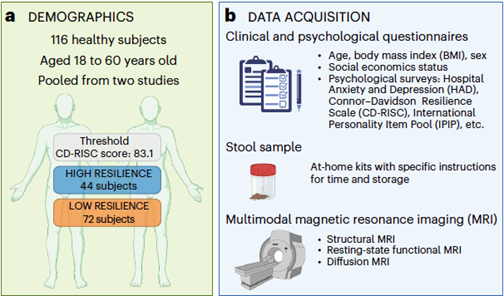
The study included 116 healthy adults aged 18 to 60. Based on their responses to a well-known psychological scale (CD-RISC), they were divided into “High Resilience” and “Low Resilience” groups. All participants completed psychological surveys, provided stool samples, and underwent detailed brain scans (MRI). Six different types of data were analyzed: psychological traits, gut bacteria taxa and function, gut-derived metabolites, and three types of brain imaging.
Resilient People Are Different—Inside and Out
At the brain level, resilient individuals showed differences in the connectivity of certain brain networks, in particular increased connectivity in networks related to emotion regulation, mindfulness, and motivation. Resilient individuals also showed less gray matter in emotion-sensitive brain areas, which might reflect greater efficiency or flexibility in handling stress. These patterns suggest that resilient people use their brains differently—more efficiently and adaptively—when dealing with emotional challenges.
At the microbiome level, resilient individuals had a gut microbiome with a greater prevalence of bacteria producing anti-inflammatory metabolites, which may send “calming” signals to the brain, strengthening emotional stability and coping ability. These molecules include short-chain fatty acids (SCFAs), like butyrate which have been shown to reduce inflammation in the body and brain, strengthen the gut lining. People with higher resilience had more bacterial pathways involved in producing these beneficial helpful compounds.
On a psychological level, resilient individuals scored lower on anxiety, depression, stress, and neuroticism, higher on traits like extraversion, mindfulness, self-awareness, and focus and better on self-reported cognitive tasks, like memory and attention. Based on these findings one can speculate that these psychological strengths likely work hand-in-hand with gut and brain biology to protect mental well-being.
What Does This Mean for You?
This research suggests that resilience isn’t just about mental toughness—it’s about a healthy partnership between your brain and your gut. This partnership implies that a balanced gut microbiome may protect your brain from the harmful effects of chronic stress. Even though reported data have mainly come from animal studies, interventions that improve gut health—like a healthy, non-inflammatory diet, certain probiotics, and better stress management might also build psychological resilience.
Takeaways for Daily Life
Here’s how you might support your brain–gut connection for greater resilience:
| Action | Why It Helps |
| Eat a variety of plant based foods, providing more fiber and fermented foods to your gut microbes | Supports bacteria that make SCFAs and reduce inflammation. |
| Regularly practice mindfulness or meditation | Boosts brain regions tied to emotion regulation. |
| Exercise regularly | Calms your immune system and promotes both microbiome diversity and brain health. |
| Sleep well | Helps regulate stress hormones and gut health. |
This is the first major study to integrate brain imaging, gut bacteria activity, and psychological testing into a single model of resilience. It shows that our ability to handle stress may be hardwired into the brain-gut microbiome system. By studying both brain structure and connectivity, microbial function and psychological traits, the authors identified a kind of “biological signature” of resilience—one that could lead to future treatments or prevention strategies for stress-related conditions.
We’ve always known that some people are better at handling stress. The UCLA study gets us a step closer to understand why: It’s not just mindset or personality—it’s biology, including your genes. Your gut microbiome might be one of your best allies in staying emotionally strong. And that means taking care of your gut microbiome could be one of the smartest ways to take care of your mind.

Emeran Mayer, MD Is a Distinguished Research Professor in the Departments of Medicine, Physiology and Psychiatry at the David Geffen School of Medicine at UCLA, the Executive Director of the G. Oppenheimer Center for Neurobiology of Stress and Resilience and the Founding Director of the Goodman-Luskin Microbiome Center at UCLA.